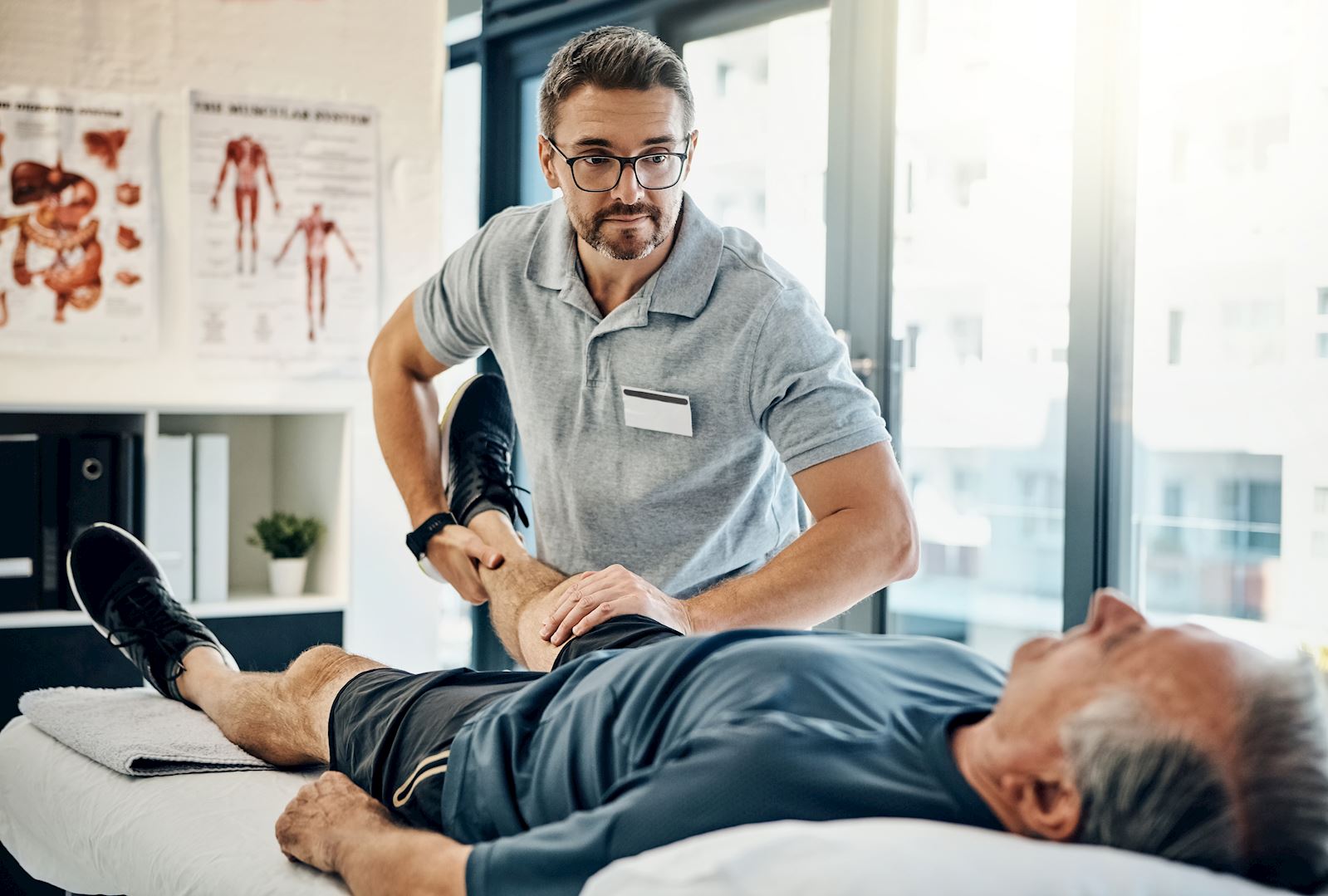
Pain Management Medical Expertise
Whether you suffer from temporary or chronic pain due to illness or injury, our pain management team will help you find the best treatment plan to find relief.

Chronic Pain Management
When you're in pain, we work to relieve it — no matter if it's a new problem or one you've been dealing with for years.
Epidurals
Injections targeting your spinal cord stop pain signals from moving throughout your body and offer long-lasting relief.
Facet, Nerve and Plexus Blocks
Blocks target specific parts of the body to relieve pain immediately and help limit it in the long run.

General Pain Management
Don't let pain stop you from your favorite daily activities. See what options are available for you, including radiofrequency ablations spinal cord stimulators, injections and more.

Joint Pain
Joint pain ranges from bothersome to debilitating. There's wide variety of treatments to relieve this range of symptoms.

Neck & Back Pain
Neck and back pain are leading causes of disability. We find where the pain comes from along your entire spine.

Spinal & Spinal Cord Issues
Pain can radiate from your spinal cord or the joints and tissue that protect it. We treat all two feet of the spine.
Find a Provider
Find Pain Management care at an Iowa Clinic location nearest to you.
Pain Management providers are conveniently located at campuses in or near the Des Moines metro area.